
In recognition of National Infertility Awareness Week, we are seeking to raise awareness about this struggle by sharing stories from local moms and a dad who have been in this difficult place, as well as additional local resources to help parents along this journey. Through this series, we hope to provide encouragement for women and men who are facing infertility and perspective for those supporting them in the battle. Thank you to our sponsors, UAB Women & Infants Services, and to each of the contributors to this series — especially the courageous parents who have shared a painful piece of your journeys.
Hello, my name is Melissa, and I am an infertility survivor. We come in many shapes and sizes, many titles and check boxes. Some of us cross the finish line with a baby (or babies) in hand. Some reroute their journey.
My journey began in 2011, when I was 29 years old. My husband and I had been married for a little over a year and were thinking about starting a family. Thirty seemed like a good age. We were in a good place in our marriage and careers but thought one more year under our belts would help.
When I visited my OB-GYN for my annual check-up, my doctor asked me about whether I wanted to have children. I did, but I wanted to wait another year. My doctor looked at me and said, “Melissa, it could take a year for you to get pregnant. You are young, but you never know.”
I laughed it off, grabbed my prescription for another year of birth control and went back to life as usual. Before I knew it, I was three months away from my 30th birthday. I read somewhere that it takes three months for birth control to get out of your system and for your cycle to start regulating, so I went off birth control. I was SURE I would get pregnant right away. I was POSITIVE! My mother had no issue getting pregnant. My maternal grandmother started having kids in her thirties. My paternal grandmother had my father (her last of six children) when she was in her mid-forties! I was made for this!
After three months, I was not pregnant. My cycle was not regulated at all.
I went back to my doctor. He could have said, “I told you so,” but he didn’t. Instead, he went into problem-solving mode. He said I might have polycystic ovarian syndrome (PCOS), meaning my ovaries develop multiple cysts which mess up my cycle. I would need a sonogram to see if this was the case.
The sonogram showed that I had some cysts on my ovaries, but not enough to diagnose me with PCOS. My doctor was still concerned. He said he thought the best move would be to start seeing a Reproductive Endocrinologist (RE).
I’ll pause here to say that MOST women do not get to this point in just three months of trying to conceive (TTC). The rule is that if you are under 35, you TTC for one year; and if you are 35 or over, you give it six months. My OB-GYN pushed for this. I pushed for this. You can push for this, if you’re in a similar situation.
In my first appointment with my RE, we went over all the tests I had to take to figure out what my issue could be. All my bloodwork came back fine, with a few exceptions that were easily regulated with medication and supplements. I was also put on metformin, a drug typically prescribed to diabetics, to help regulate my cycle.
The final test was an invasive one: a hysterosalpingogram, or HSG. During the HSG, they shoot dye through your uterus. If things are normal, it should escape through your fallopian tubes. Things went swimmingly with my right tube. My left tube was another story. It was closed off. Because I could see the entire test on a TV monitor, I got to watch my tube swell with dye, live. My doctor said I had to have this closed-up tube removed if I wanted to get pregnant.
My RE and I now had a game plan. Remove the tube, get on some good old-fashioned infertility meds and make a baby! I had the surgery. All went well. My RE said I should take a few months off to heal and relax before starting the meds.
Before we could even try the meds, it happened. I was pregnant! My husband and I were on cloud nine.
At our six-week ultrasound, we got bad news. Our baby was not measuring where it should be. There was just a 50% chance this pregnancy would continue. We were told to come back in two weeks.
The day of that next appointment is still hard to think about. That morning, we found out my husband’s grandfather died. Later that day, we learned we had also lost the baby.
The year that followed was filled with infertility meds, injections, cycle tracking, tears, arguments, pain, isolation, emotions, vaginal ultrasounds, an unsuccessful attempt at intrauterine insemination (IUI), hormonal mood swings, and RE appointments. LOTS of RE appointments. We even sat through an intense meeting about in-vitro fertilization (IVF).
We took a month off the meds toward the end of the year because pumping my body full of hormones made another pesky cyst appear. I went off the meds and guess what? Pregnant again!
We didn’t even make it to the six-week ultrasound before losing the baby.
 We were not messing around anymore. After the first of the year, we dove head-first into IVF. I could write a book on the whole IVF process, but here it is in a nutshell.
We were not messing around anymore. After the first of the year, we dove head-first into IVF. I could write a book on the whole IVF process, but here it is in a nutshell.
- We retrieved seven healthy looking eggs after weeks of meds designed to increase “egg production”.
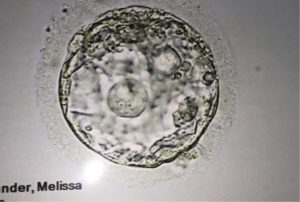
- Four of those eggs made it to the blastocyst stage, which is typically a five-day-old embryo.
- We had the blastocysts genetically tested because of my recurrent miscarriages. Only ONE was healthy enough to make it a full term.
Everything was riding on this ONE little guy (we got to find out the gender super early thanks to the genetic screening). While there is no way to know for certain, my RE thinks this is a sign my eggs are aging faster than my body. This might be our only shot at a pregnancy.
 Thirty-five weeks after transfer, Nicholas entered our world. His birth story has its own set of twists and turns that are perfect for another story. Today, we have a two-year-old tornado with dark brown hair tearing through our house. All the tears and pain we felt over nearly three years has buried itself in the back of our heads. For us, the struggle was worth it.
Thirty-five weeks after transfer, Nicholas entered our world. His birth story has its own set of twists and turns that are perfect for another story. Today, we have a two-year-old tornado with dark brown hair tearing through our house. All the tears and pain we felt over nearly three years has buried itself in the back of our heads. For us, the struggle was worth it.
That struggle does not always end the way ours did. Sometimes the first round of IVF doesn’t work. Sometimes rounds two through seven don’t work. And, sometimes you have a handful of perfect little embies that you can come back to down the road.
The bottom line is that infertility is HARD. You could be 25, 30, 40 – whatever age you are, it is hard. It sucks. It beats you down. It isolates you. Reproduction is something that your body was designed to do, and when you can’t do it, you feel defeated and not human. This process comes with a mixed bag of emotions and problems that is different for everyone it’s handed to. If you are going through it, I am sending you the biggest virtual hug right now. If you know someone who is going through it, cut them some slack, lend them an ear, and understand that any anger, mood swings, and sensitivities are a result of this ferocious beast that they feel like they’re battling alone.
 Melissa is a full-time working mother who lives with her husband, “two-year-old tornado” and a precocious pup. She loves Walt Disney World and giving vacation tips to moms planning trips to the “house of the mouse.” Melissa has always related to elephants because she never forgets (unless it’s the laundry that needed to be moved to the dryer or an extra binky for the road). She also has an unhealthy obsession with her Instant Pot and loves when her Pinterest recipes come out better than she imagined! She swears she’ll find a workout routine she can stick with . . . eventually.
Melissa is a full-time working mother who lives with her husband, “two-year-old tornado” and a precocious pup. She loves Walt Disney World and giving vacation tips to moms planning trips to the “house of the mouse.” Melissa has always related to elephants because she never forgets (unless it’s the laundry that needed to be moved to the dryer or an extra binky for the road). She also has an unhealthy obsession with her Instant Pot and loves when her Pinterest recipes come out better than she imagined! She swears she’ll find a workout routine she can stick with . . . eventually.











