It runs in my family.
My granddad had it and so does my first cousin. In fact, my parents were on alert throughout my entire childhood, carefully watching (waiting?) to see the symptoms emerge for me and my siblings. Thankfully, in those younger years, the symptoms never came. Aside from the occasional virus or sinus infection, all of us were healthy overall. When we kiddos reached our teenage and young adult years . . . just as we presumed everyone was out of the woods . . .
I became the “lucky” one.

Type 1 diabetes (T1D) is a chronic autoimmune disease that is developed mostly due to genetic predispositions, and has nothing to do with lifestyle or diet choices, as is the typical (false) understanding within the general public. Its onset begins when the body attacks its own pancreas, shutting down beta cell production and function and forever damaging and obliterating the pancreas’ ability to create insulin. In short: my pancreas is useless because my own body attacked itself and shut it down. I do not make my own insulin, and nothing I do can awaken insulin production, so I must administer insulin manually. We’ll get there in a minute. T1D is relentless, life-threatening, and has no cure. Our culture perpetuates many harmful misconceptions about diabetes as a whole, and Type 1 hardly fits into any of them; it’s an entirely misunderstood beast of its own.
My Diagnosis Story
My first week of college classes, I randomly became ill; it was the sickest I had ever been up until that point. I was a Vocal Music Education major and my voice was crucial to succeeding in my classes. You could imagine my frustration at the sudden inability to rely on my body. From August to December of that year, I battled tonsillitis nine times. Once my tonsils were removed at the end of December, I thought that would be the end of my health journey and I could move forward with my degree and my life.
Unfortunately, this was only the beginning.
The Early Signs
The following two years consisted of one health flareup after another. Once one issue would be resolved, something else came along. They were all weird infections that required different specialists, but not one of these specialists thought to run a HbA1c test on me. (The HbA1c tells you what your blood sugar has been running for the past three months.)
It was mid-May of 2013. I had just wrapped up finals week and headed home to my parents’ house here in Birmingham (I attended college in Ohio.) Mom picked me up, and we drove nine hours to get back to Birmingham. Every hour or so, we had to pull over for me to use the restroom. I was drinking so much water throughout the trip (my thirst was never quenched), so I assumed that’s why I needed to stop so much. I also struggled to read the big directional signs on the interstate (they were suddenly super blurry), but I chalked that up to an outdated contact prescription – who has time to take 24 semester credit hours AND go to the eye doctor?
A few days after being home, I remember my mama talking about how trim I was looking, which made me happy since I was in the midst of planning my wedding and was working hard to look good in my wedding dress. I didn’t have a scale in my room at school and didn’t know how much I weighed. I remember weighing myself on my parents’ bathroom scale and being shocked at how low the number was. I attributed it to wedding planning, finals week, and hustling to finish my degree.
Over the next few days, my mom and I kept talking about the random weird symptoms I had been experiencing as of late. We thought I was on the cusp of another curious medical issue. That was the understatement of the year. I wasn’t as familiar with T1 symptoms as my parents were, since they were constantly on the lookout for them throughout all of our childhoods. I’m not sure what it was, but something provoked me to ask during our conversation, “Does this sound like the symptoms of type 1 diabetes?”
I will never forget the look on her face. It was a stark look of realization, fear, and sadness all in one.
Looking for Answers
We got an at-home HbA1c test kit just to “rule it out”. We were hoping for a number under 5 (meaning non-diabetic levels.) After a few finger-prick attempts and five minutes, 9.6 flashed on the screen. We didn’t know what else to do, so she took me to the ER. I kept feeling so weird about going because I didn’t look sick, but in we went. They tested my blood sugar while checking me in, and I was immediately triaged with a blood sugar nearing 500 (normal range is 80-120.) After hours of lab work and waiting, the doctor came in to confirm our fears:
Type 1 diabetes.
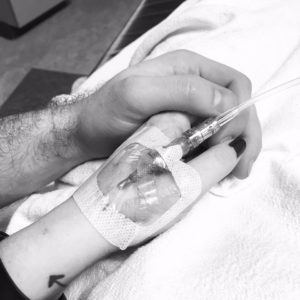
A New Life
The doctor and nurses were trying to convince me to be admitted, but I was planning to go back to work later in the week and refused (not realizing what a terrible decision that was.) My soon-to-be husband was out of the country for a few weeks and wasn’t available to help talk me into being admitted. They agreed to release me if I promised to return to the hospital the following afternoon for an invasive appointment and education session on how to dose for insulin and to schedule a follow up with a doctor in my college town when I returned home. Type 1 diabetics require insulin for survival. No amount of lifestyle change will impact this disease; it is incurable and life-threatening.
Because I was determined to not allow T1D to rule me or thwart my plans, I jumped right back in to school, work, and life. In retrospect, I wish I would have listened to the staff the night of my diagnosis and just let myself be admitted. I have had to learn how to understand and live with T1 mostly on my own. I’ll never forget how terrible I felt the first few days of insulin injections. My body got used to functioning without insulin (living unknowingly and dangerously hyperglycemic), and adding it back in was a shock to my system. Once my body got used to having insulin again, I was shocked at how much better I felt; I had been in survival mode without insulin, not realizing how badly I was feeling.
Not So “Juvenile”
I was 20 when I was diagnosed with a “juvenile” disease. Type 1 is mostly diagnosed in childhood years and is sometimes referred to as “juvenile diabetes,” although that is now considered an outdated phrase. When you have the genetic predisposition for type 1 diabetes, it can present itself anytime, but it happens most often either in childhood (the most common time) or in young adulthood. We never knew about the window in young adulthood, so T1 was not on our radar anymore. It is now, for my siblings and my own children.
Something non-diabetics love to say when you’re diagnosed with type 1 is: “Well, at least it’s something manageable.” I would nod in agreement in the early days, not knowing how inaccurate this statement is. T1 is thankfully not terminal, but it is certainly not manageable. This disease has tried to take my life multiple times thanks to diabetic ketoacidosis (DKA). Most people from the outside don’t understand the seriousness and reality of what T1Ds have to deal with. It’s our normal, and we have no choice but to keep on going. Some days, T1 responds exactly the way you plan and wish for, and other days, you do everything exactly “right” and it spirals out of control regardless. All you can do is the best you can do; T1 is going to do whatever it wants to. But at least you know you’ve done your best.
Daily Fighter
My life now revolves around an ever-beeping insulin pump, sensor (continuous glucose monitor), pump site changes, injections when needed, and the constant mitigation of forever-fluctuating blood sugar levels. My days are now measured by site-change-days instead of days of the week. I’m a completely different person than I was pre-diagnosis. I lived 20 years of life without a chronic disease, and I remember vividly what it was like. I do miss those days, but I also know I wouldn’t be half the woman I am without acquiring the resiliency and determination that a life with type 1 diabetes provides. I am grateful to have a patient, involved toddler who isn’t afraid of watching me change sites and who graciously waits as I tend to my emergency blood sugars before being able to tend to her. Having a strong support system is vital for a type 1 diabetic, and I’ve got the best.

**Type 1 diabetes symptoms are frequently confused with flu-like symptoms. Please stay alert and in tune to the following symptoms as we enter flu season: increased thirst, frequent urination, bed-wetting in children who previously didn’t wet the bed during the night, extreme hunger, unintended weight loss, irritability and other mood changes, fatigue and weakness, blurred vision. If you suspect that you or your child may be exhibiting early signs of type 1 diabetes, please consult your doctor right away.














My daughter was 15. She looked like she had red socks on. Her bg was 737 when diagnosed. Her blood was so sludgy, which is why her feet were red. It wasnt until they put her into intensive care that I realized this is serious. Thankful for the progress in this field.
Comments are closed.